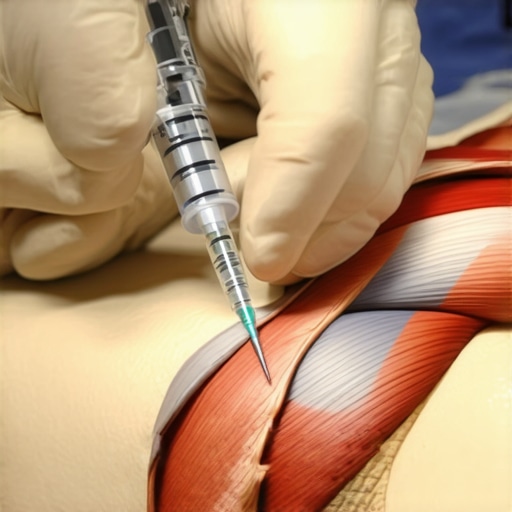
I remember it vividly—a long day at my desk, shoulders tense, neck aching, and that familiar, nagging pain creeping up my spine. I ignored it at first, thinking it was just stress or fatigue. But days turned into weeks, and the discomfort became a constant companion, stealing my focus and draining my energy. I found myself questioning whether I needed a spine surgeon, a chiropractor, or just more rest. That lightbulb moment hit me hard—there had to be a better way to tackle this persistent muscle pain, one that didn’t involve invasive surgery or a lifetime of medication.
Discovering the Power of Trigger Point Injections
What really transformed my understanding was learning about *trigger point injections*—a minimally invasive treatment targeting stubborn muscle knots that cause relentless pain. These injections deliver medicine directly into the tight, tender spots, helping muscles relax and pain diminish. Many people, like myself, initially dismiss this option, thinking it’s just another fad or unnecessary fear. But after experiencing relief firsthand, I knew I had stumbled upon a genuinely effective solution. Today, I want to share what I’ve learned so you don’t have to suffer in silence or jump straight into more drastic measures.
Is Trigger Point Therapy Actually Worth the Hype?
Early on, I made the mistake of assuming all treatments are created equal. I hesitated, thinking, “Will this really work for my chronic muscle pain?” It’s a common doubt. But understanding that these injections are backed by scientific studies—as supported by experts like those at NJ Orthopedic—helped me make an informed decision. If you’re tired of living with nagging pain and tired of trial-and-error, I invite you to explore this promising approach. The journey from constant discomfort to relief isn’t always straightforward, but with the right knowledge, you can take control of your muscle health. Next, I’ll walk you through what to expect from trigger point injections and how to decide if this is the right step for you.
Start with a Precise Diagnostic
Before any treatment, schedule a comprehensive orthopedic evaluation to identify the exact muscles causing pain. Think of this step as plotting your GPS before a road trip; it ensures you head in the right direction. During your appointment, expect your doctor to perform physical exams and may recommend imaging or nerve tests if needed. For instance, if numbness accompanies pain, a nerve test might be essential—learn more about nerve tests at this resource.
Learn What Trigger Point Therapy Can Do
Understanding the core concept of trigger point injections is crucial. These injections neutralize muscle knots—think of them as relieving a cramp that’s been stubbornly staying put. The procedure involves injecting medicine directly into the tender spots, which relaxes the muscle fibers and alleviates pain. You might compare it to unwinding a tightly coiled spring—once relaxed, movement becomes easier, and discomfort diminishes. For an in-depth look at how these minimally invasive treatments work, visit this page.
Decide if Injections Are Suitable for You
Evaluate whether trigger point injections align with your condition. If your pain is localized and persistent, this approach often offers relief without surgery. A consultation with an orthopedic specialist will help determine candidacy. Be prepared to discuss your medical history, previous treatments, and pain patterns. For example, during my own consultation, I noted that my muscles were consistently tense in the shoulder blade area—indicating trigger points. My doctor explained that this targeted treatment could relax those knots effectively.
Prepare for the Procedure
Understanding what to expect can lessen anxiety. The injection is quick—often taking less than 30 minutes—and typically performed under local anesthesia. During the process, you’ll feel a small needle prick, similar to having a blood test. Afterward, some soreness might occur, but it usually resolves within a day. I recall a time when I had a mild discomfort afterward; applying ice helped manage it. Rest assured, most patients experience significant relief within a few days.
Post-Treatment Care and Monitoring
Effective recovery involves following your doctor’s instructions closely. Mild soreness can be alleviated with over-the-counter pain relievers and stretching exercises. For guidance on orthopedic rehabilitation after injections, see this guide. Keep track of your pain levels and report any unusual symptoms—such as increased swelling or persistent numbness—to your clinician promptly. Regular follow-up appointments ensure the treatment is progressing as intended.
Consider Additional Lifestyle Changes
Integrate ergonomic adjustments into your daily routine, like proper desk setup and regular breaks. Strengthening and stretching exercises can support the healing process and prevent future muscle knots. For specific exercises suited for desk workers, explore tips at this page. My own experience shows that combining injections with physical therapy and posture modifications yields the best results.
Know When to Escalate Your Care
If pain persists beyond a few weeks or worsens, consulting an orthopedic surgeon or a specialist in spine health may be necessary. Sometimes, these injections are part of a larger treatment plan, including therapies or surgical consultation—especially if structural issues like scoliosis or spondylolisthesis are involved. Explore how to choose the right surgeon at this resource or review top specialists at this list.
Many assume that visiting an orthopedic specialist is straightforward, believing any consultation or diagnosis is a simple step toward relief. However, the landscape is riddled with nuances, myths, and common mistakes that can hinder effective treatment, especially for desk workers dealing with chronic back pain. Let’s unravel some misconceptions and shed light on what truly goes on behind the scenes.
One prevalent myth is the belief that a general practitioner or even a chiropractor can adequately address complex orthopedic issues without specialized input. While these providers are valuable, they often lack the diagnostic tools to identify subtle structural problems, such as spondylolisthesis or scoliosis, which require detailed imaging and specific coding. Understanding the **common orthopedic diagnosis codes**—like M51.36 for lumbar spondylolisthesis or M54.5 for low back pain—can empower patients to advocate effectively during their visits. Familiarity with these codes also helps in insurance claims and treatment planning.
Another mistake is the assumption that all back pain originates from spinal issues needing a spine surgeon. Sometimes, a consultation with an orthopedic doctor suffices and can exclude the need for invasive procedures. Experts suggest that, unless imaging reveals severe structural damage or nerve impingement, conservative treatments like minimally invasive injections might offer relief. For example, [this](https://njorthopedicdoctor.xyz/minimally-invasive-back-pain-treatments-explained) resource discusses how non-surgical interventions often outperform assumptions about surgery being the default.
Advanced readers might ask:
Should I see an orthopedic doctor or a neurologist for my chronic back pain?
The answer depends on your symptoms. While neurologists specialize in nerve-related issues, orthopedic doctors are trained to evaluate musculoskeletal causes. Misdiagnosing or choosing the wrong specialist can lead to delays, unnecessary procedures, or exacerbated pain. For persistent, localized pain without neurological deficits, an orthopedic consultation is often more appropriate. Learn what to expect during your appointment at [here](https://njorthopedicdoctor.xyz/what-to-expect-at-your-first-orthopedic-consultation-in-2026-2).
Beware the trap of over-relying on imaging too early. Vague or incidental findings can lead to unnecessary surgeries or treatments. Experts advise targeting diagnostic clarity through thorough clinical exams first, reserving imaging for when it’s truly justified. This approach aligns with conservative, effective management strategies emphasized in [this](https://njorthopedicdoctor.xyz/orthopedic-vs-neurosurgeon-for-spine-4-facts-for-your-2026-surgery) overview.
Lastly, neglecting lifestyle factors is a common oversight. Ergonomic assessments and targeted physical therapy are crucial components of a holistic treatment plan. For desk workers, simple adjustments can prevent future issues, as discussed in [this](https://njorthopedicdoctor.xyz/5-orthopedic-tips-for-desk-workers-to-fix-2026-lower-back-pain) article.
In summary, navigating the orthopedic landscape demands awareness of diagnostic coding, appropriate specialist selection, and cautious interpretation of imaging. Don’t fall into the trap of thinking that all solutions are surgical or immediate. Instead, adopt a nuanced view that balances conservative treatments with precise diagnostics. Have you ever fallen into this trap? Let me know in the comments.
Keeping It Working: Tools I Recommend for Orthopedic Wellness
Maintaining orthopedic health over time requires a balanced combination of effective tools, proper habits, and proactive management. For desk workers, I personally rely on ergonomic equipment such as an adjustable standing desk, which allows me to alternate between sitting and standing, reducing spinal strain. An ergonomic chair with lumbar support ensures proper posture during prolonged periods seated. Additionally, foam rollers and massage balls have become indispensable for my daily stretching routines, helping to release muscle knots and improve flexibility. This resource highlights how minimally invasive treatments complement physical tools for sustained relief.
On the software side, I utilize posture tracking applications like Upright or Lumo to receive real-time feedback and alerts when my posture deviates from optimal alignment. These tools serve as constant reminders to correct my position, preventing chronic issues. Incorporating wearable devices, such as a fitbit or Apple Watch, encourages regular movement and breaks, which are critical in avoiding stiffness and muscle fatigue. My experience confirms that consistent micro-movements significantly impact long-term spinal health.
Prediction for the Future of Orthopedic Maintenance
Looking ahead, I believe the integration of AI-driven posture correction systems and smart furniture will revolutionize how we maintain spinal health daily. Virtual physiotherapy sessions, guided by data from wearable devices, will become more accessible, making preventive care routine rather than reactive. Continuous advancements suggest that people will have personalized, tech-enabled solutions tailored specifically to their movement patterns and structural needs.
How do I maintain my orthopedic health over time?
The key is consistency in using the right tools and adhering to recommended habits. Supplementing ergonomic equipment with targeted exercises—like the stretching routines detailed in orthopedic rehab tips—can drastically reduce the risk of chronic pain development. Scheduling regular check-ins with an orthopedic specialist ensures your approach evolves with your needs rather than becoming stagnant. Remember, proactive intervention and staying informed about new technologies can keep your spine healthy and functional for years to come. Don’t hesitate to try out one of these advanced tools and observe how it enhances your daily routine.
Throughout my journey with chronic muscle pain, I realized that the most valuable lessons often come from unexpected sources. One of the hardest truths I discovered was that quick fixes rarely address the root cause of musculoskeletal issues. Embracing detailed diagnostics and seeking specialized guidance made all the difference. It became clear that arming myself with knowledge—about diagnostic codes, treatment options, and when to escalate care—was essential in navigating the complex world of orthopedic health. That lightbulb moment taught me to listen more carefully to my body and trust the process of targeted, informed treatment.
Another insight was realizing the power of combining minimally invasive therapies like trigger point injections with lifestyle modifications and ergonomic adjustments. Small daily habits—like proper posture and regular movement—compound over time into significant relief and improved function. I also learned that finding the right specialist, whether it’s an orthopedic doctor or a spine surgeon, depends on understanding your specific condition and goals. This personalized approach can prevent unnecessary treatments and foster confidence in your recovery path.
Finally, staying proactive and curious about emerging treatments can open new doors. Technologies like AI-powered posture correction or advanced physical therapy programs are reshaping how we maintain spinal health. The key takeaway is that comprehensive, patient-centered care—paired with ongoing preventive habits—powers sustainable relief and wellness. Embrace your journey, seek tailored solutions, and remember: the road to orthopedic health is a marathon, not a sprint.