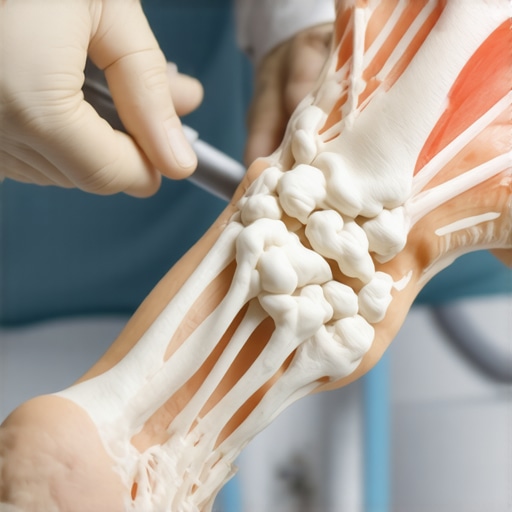
It was the moment I dreaded most—trying to walk after spraining my ankle during a weekend hike, only to realize that the pain was far worse than any typical sprain. I remember limping back to my car, feeling that gnawing worry creeping in: was this really just a twist, or could I have fractured something? That experience taught me a crucial lesson: not every ankle pain is what it seems, and rushing to dismiss it as a simple sprain can lead to long-term issues.
Don’t Underestimate the Seriousness of Ankle Injuries
Many people assume that if an ankle hurts and swelling goes down, they’re in the clear. But here’s the truth—some ankle fractures are sneaky. They might initially feel like a bad sprain, but over time, improper healing can cause chronic instability, arthritis, or even deformity. I learned this firsthand when a client shared her story; she ignored the pain, convinced it was just a sprain, only to face a more complicated recovery later because a fracture was missed in the first assessment.
Did you know that up to 70% of ankle fractures require surgical intervention, especially if diagnoses are delayed or missed? (Source: American Academy of Orthopaedic Surgeons). This staggering number highlights the importance of not brushing off significant ankle injuries.
**So, what’s the key?** It’s understanding why a proper evaluation matters and when to see a specialist—because knowing the difference can change everything.
What We’ll Cover Today
In this post, I’ll share practical insights based on personal experience and expert knowledge. We’ll discuss how to recognize signs that your ankle injury might be more serious than a sprain, what steps to take immediately, and why consulting an orthopedic specialist isn’t just a good idea—it’s essential to ensure proper healing and avoid unnecessary complications.
Now, I want to ask—have you ever injured your ankle and thought, “It’s just a sprain,” only to find out later it was something more serious? If so, keep reading, because understanding the right approach can save you pain, time, and money in the long run.
By the end of this guide, you’ll know exactly when to seek professional care and how an orthopedic expert can make all the difference in your recovery journey. Ready to find out what you might be missing? Let’s dive in.
Perform an Immediate Self-Check
Start by evaluating the severity of your injury. Compare your pain and swelling to a familiar activity—if walking feels like trying to walk on broken glass, or if there’s a deformity, consider it a red flag. Imagine your ankle as a fragile ceramic vase; any distortion or extreme pain indicates possible structural damage that needs professional attention.
Assess Weight-Bearing Ability
Try to put weight on the injured foot. If weight-bearing worsens pain or makes your ankle feel unstable, don’t push through it. This step is like testing the stability of a dangling chandelier—you don’t want to jar it further.
Check for Visible Deformity and Swelling
Look for obvious deformity, bruising, or swelling that resembles a balloon popping. These signs suggest a fracture or severe sprain. Remember, a simple sprain typically won’t cause a significant deformity, but a displaced fracture might.
Opt for Appropriate Imaging
If your self-assessment indicates serious injury—such as inability to walk, deformity, or severe pain—it’s critical to get imaging. An X-ray is the initial step, like opening the hood of a car to find if the engine is broken. Sometimes, an MRI might be necessary to reveal ligament tears or subtle fractures that aren’t visible on X-ray.
Why MRI and X-Ray Matters
Choosing the right scan can prevent misdiagnosis. An MRI provides detailed images of soft tissues, which is crucial if ligament injuries are suspected, while X-rays show bone fractures clearly. Knowing which to request can make a significant difference in your recovery. Read more about MRI or X-ray first.
Seek Professional Evaluation Quickly
Don’t delay seeing a specialized orthopedic doctor, especially if signs point toward a fracture or ligament tear. An experienced clinician will perform a comprehensive physical exam, comparing your injured ankle to the uninjured side—like a tailor measuring fabric for perfect fit. This step ensures you don’t dismiss serious injuries.
Understanding the Exam Process
During the exam, the doctor will test range of motion, stability, and tenderness. They may compare ligament integrity to a “shock absorber” system—if one is compromised, your ankle’s ability to absorb impact is affected, risking long-term problems like instability or arthritis. This can be likened to checking the suspension system of a car after an accident.
Decide on Treatment Strategy
If a fracture is confirmed, immobilization through casting or surgical fixation might be necessary. For ligament sprains, conservative treatments such as rest, ice, compression, and elevation—commonly known as RICE—are effective. For persistent or severe cases, consult a specialist about options like minimally invasive procedures or physical therapy, including tailored rehab programs available here.
Follow Up and Rehab
Once treatment begins, consistent follow-up is vital. Think of your recovery like rebuilding a house—careful inspection and gradual reinforcement prevent future collapse. An orthopedic rehab plan ensures your ankle regains strength and function, reducing the risk of chronic instability or arthritis later on.
Remember, recognizing red flags early and acting swiftly can save your mobility and prevent long-term disability. If you’re ever uncertain, consulting a trusted spine specialist in New Jersey can make all the difference.
 Many patients believe that all spine pain or injuries are straightforward to diagnose and treat, but the reality is far more complex. For example, a common misconception is that a bulging disc or sciatica will always cause predictable symptoms. In truth, individual anatomy and biomechanics significantly influence presentation, making diagnosis more nuanced than often assumed. Recognizing this is key to effective treatment, preventing unnecessary procedures, and setting realistic expectations.
Many patients believe that all spine pain or injuries are straightforward to diagnose and treat, but the reality is far more complex. For example, a common misconception is that a bulging disc or sciatica will always cause predictable symptoms. In truth, individual anatomy and biomechanics significantly influence presentation, making diagnosis more nuanced than often assumed. Recognizing this is key to effective treatment, preventing unnecessary procedures, and setting realistic expectations.
Why Relying Solely on Imaging Can Be Deceptive
While MRI and X-ray imaging are invaluable, they are not infallible. Studies reveal that many asymptomatic individuals show disc herniations or degenerations on imaging, yet have no pain or functional impairment—highlighting that imaging findings alone shouldn’t dictate treatment decisions. As such, an expert orthopedic exam after a car crash goes beyond looking at scans; it assesses functional deficits and biomechanics to uncover hidden issues that images might miss. Avoid the trap of over-reliance on scans by consulting a specialist who can interpret results within the broader clinical context.
Choosing Between Orthopedic and Neurosurgical Care
Many patients wonder whether they should see an orthopedic spine specialist or a neurosurgeon. While both are highly skilled, their focus differs: orthopedists often excel in structural and musculoskeletal issues, employing minimally invasive techniques when appropriate, whereas neurosurgeons typically handle complex nerve-related surgeries. Knowing the difference—and selecting the right specialist—can influence outcomes. For example, when dealing with a slipped disc, an orthopedic doctor with expertise in non-surgical and minimally invasive treatments may be the right choice. Want to learn more about picking the right spine doctor? Browse our comprehensive guide on how to choose a spine doctor, to make an informed decision.
Addressing Common Myths and Advanced Mistakes
It’s a myth that all neck or back pain requires surgery. Often, conservative management like physical therapy, targeted injections, or lifestyle modifications suffices—yet many fall into the trap of unnecessary surgical consultations early on. Conversely, delaying intervention when necessary can lead to chronic issues such as instability or nerve damage. An advanced mistake is ignoring subtle signs like persistent numbness or weakness after a work injury; these require prompt assessment by a qualified orthopedic specialist. Remember, a thorough orthopedic checklist after a work injury can uncover underlying pathology before it worsens. For expert advice tailored to your situation, consider consulting specialists listed on top orthopedic spine specialists in your area.
Have you ever fallen into this trap? Let me know in the comments. Navigating orthopedic spinal issues demands a nuanced understanding and a trusted clinical partner. When in doubt, always seek an experienced specialist who considers the full clinical picture, beyond just scans or common assumptions. Proper care can prevent long-term disabilities and help you regain mobility and comfort faster than you think.Maintaining spinal health over time requires more than just occasional visits to your doctor; it involves adopting specific tools, habits, and methods that support your spine’s integrity daily. One essential device I personally recommend is a high-quality ergonomic lumbar support pillow. Unlike generic cushions, my choice is a memory foam lumbar roll with adjustable straps, which I use during long work hours on my desk. This particular support ensures proper pelvic alignment, reducing undue pressure on the lumbar discs and preventing sciatica flare-ups. Regular use of such support has helped me avoid chronic low back pain, especially after a lumbar fusion, which necessitates careful monitoring and supportive tools for long-term success (rehabilitation tips).
Technology also plays a pivotal role in spinal maintenance. I utilize posture tracking apps like “Upright” or “Lumo Lift,” which provide real-time feedback on my sitting and standing habits. These apps connect to my smartphone, alerting me when I slouch or maintain poor posture for too long. This immediate feedback loop helps reprogram my habits, reinforcing spinal health. In fact, recent studies suggest that consistent posture correction can significantly decrease the likelihood of developing degenerative disc issues (study link).
Another practical tool is foam rolling and myofascial release devices such as a Theracane or a massage foam roller, which I use to maintain flexibility and release muscle tension around my spine. Keeping the paraspinal muscles supple prevents long-term biomechanical imbalances that could lead to issues like cervical or lumbar disc bulges. Incorporating daily stretching routines with these tools is a game-changer in my ongoing prevention regimen.
Looking ahead, the trend in spinal care is leaning toward **smart wearable technology** that continuously monitors spinal biomechanics and provides personalized recommendations. Companies are developing sensors that detect subtle postural deviations or early signs of disc degeneration, empowering users to take proactive measures. As these technologies improve, they will likely become standard in maintaining spinal health for at-risk populations.
**How do I maintain long-term spine health as I age?** Regularly use ergonomic supports during daily activities, leverage posture correction apps for immediate feedback, and incorporate myofascial tools like foam rollers into your routine. Remember, prevention begins with consistent habits—small daily actions can prevent significant issues later. If you’re unsure about best practices, consulting with a spine specialist can provide tailored guidance. To find experienced professionals, visit our recommended list of top specialists. Don’t wait for pain to take hold—start integrating these tools today and keep your spine working for years to come.
What the Experts Won’t Tell You About Spinal Healing
One profound lesson I learned is that sometimes, the biggest breakthroughs come from acknowledging what we don’t know—and then actively seeking expert insights. I once dismissed subtle signs of a disc herniation, thinking rest would suffice, only to realize that early intervention with a specialist could have prevented months of unnecessary pain. This realization taught me to trust not only my instincts but also the nuanced guidance of seasoned spine professionals, who see beyond the scans and listen to the story your body tells. Remember, sometimes the path to recovery involves unlearning assumptions and embracing expert advice that challenges the status quo.
Curated Tools That Keep Your Spine Strong
Over the years, I’ve found that investing in ergonomic tools like a memory foam lumbar support pillow can make a world of difference, especially during long work hours. Paired with posture tracking apps such as “Upright,” I stay conscious of my sitting habits, reducing strain on my cervical and lumbar regions. Additionally, incorporating foam rollers like a Theracane into my daily routine helps release muscle tension, preventing biomechanical imbalances that could exacerbate issues like sciatica. For anyone serious about lasting spinal health, these tools aren’t just accessories—they’re essential allies in your wellness journey. Learn more about effective non-surgical care options for herniated discs and how tailored strategies can prevent chronic pain.
Your Next Step for Wellness Starts Today
Healing and maintaining your spine’s health is a continuous journey, not a one-time fix. By trusting your body, leveraging expert insights, and adopting proactive tools, you set the foundation for a pain-free future. Remember, you have the power to influence your spinal health through everyday habits and informed choices. Whether you’re dealing with sitting-related discomfort or recovering from a recent injury, taking action today can redefine your tomorrow. Dive into our comprehensive resources, and don’t hesitate to reach out to top specialists in New Jersey who can guide you with personalized care. Your spine deserves it—start now, and embrace a life of mobility and comfort.
Have you ever overlooked early signs of a spinal issue? Share your experience below and let’s learn from each other’s journeys to better health.