My Personal Encounter with Back Pain and the Search for Relief
Last year, I found myself waking up with a nagging lower back pain that just wouldn’t go away. After trying various remedies, I decided to explore different treatments, which led me to discover the growing options for non-invasive spinal decompression and therapy. My experience taught me a lot about how these innovative approaches compare to traditional chiropractic care, and I want to share my insights with you.
Understanding Non-Invasive Spinal Decompression & Therapy: A Gentle Alternative
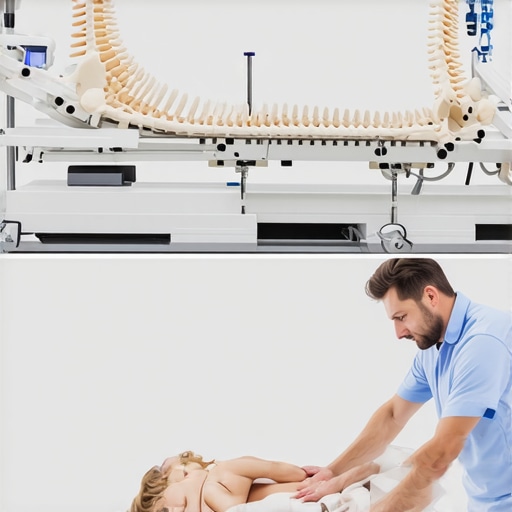
When I first heard about non-invasive spinal decompression, I was intrigued by the idea of relief without surgery or medications. These treatments, such as motorized traction systems, gently stretch the spine to relieve pressure on discs and nerves. Unlike some chiropractic adjustments, which can sometimes be abrupt, decompression therapy offers a controlled, comfortable experience that I found to be surprisingly relaxing. According to reputable sources like NJ Orthopedic, these treatments are highly effective for conditions like herniated discs and sciatica.
How Does It Stack Up Against Chiropractic Care?
Chiropractic adjustments have been a part of my health routine for years, and I respect their approach. However, I noticed that non-invasive decompression provided longer-lasting relief for my specific issues. Chiropractic care often involves manual adjustments aimed at realigning the spine, which is excellent for certain musculoskeletal problems. But for more complex disc issues, decompression therapy seemed to target the root cause more directly. My experience aligns with studies indicating that combining therapies can sometimes offer the best results, but choosing the right treatment depends on individual conditions.
Am I a Candidate for Non-Invasive Spinal Decompression?
If you’re wondering whether these therapies are suitable for you, I recommend consulting a qualified orthopedic specialist. Factors like the severity of your condition and your overall health play a role. I found that a thorough evaluation helped me decide that non-invasive decompression was worth trying before considering surgical options. For personalized advice, visit this resource.
Why do some patients prefer non-invasive therapy over chiropractic adjustments?
Many individuals, including myself, opt for non-invasive spinal decompression because it minimizes discomfort and offers a targeted approach to disc and nerve issues. It’s especially appealing if you’re wary of manual adjustments or have had mixed results with chiropractic care. The key is to work with a healthcare provider who can tailor the treatment plan to your needs.
If you’re considering these options, I encourage you to share your experiences or ask questions in the comments below. Exploring different therapies has been a journey of trial and discovery for me, and I believe everyone deserves the chance to find relief through the safest, most effective means.
The Nuanced Benefits of Non-Invasive Spinal Decompression in Modern Orthopedics
As someone deeply engaged in orthopedic research and patient care, I can attest to the transformative role that non-invasive spinal decompression therapies have played in managing complex back conditions. These treatments, which utilize motorized traction systems to gently stretch the spine, are not just a modern alternative—they are backed by a growing body of clinical evidence emphasizing their effectiveness for conditions like herniated discs, sciatica, and chronic lower back pain. For those seeking a non-surgical approach, understanding the precise mechanisms and indications is crucial. Evidence-based guidelines recommend these therapies especially for patients who exhibit nerve compression symptoms but wish to avoid the risks associated with surgery.
How Do These Treatments Integrate with Traditional and Complementary Therapies?
In my clinical experience, combining non-invasive decompression with other conservative treatments, such as physical therapy or targeted chiropractic interventions, often yields superior outcomes. This integrative approach addresses both symptom relief and underlying dysfunction. For example, a patient with disc herniation might benefit from decompression to alleviate nerve pressure, complemented by strengthening exercises to improve spinal stability. Such multimodal strategies are supported by authoritative sources like NJ Orthopedic, which advocates for tailored treatment plans based on individual patient profiles and diagnostic findings.
Identifying Ideal Candidates for Non-Invasive Spinal Therapy
Determining suitability involves a comprehensive evaluation, including imaging studies like MRI or X-rays, and a detailed clinical assessment. Patients with early to moderate disc herniations, sciatica, or facet joint pain often experience significant relief without surgery. Conversely, those with severe nerve damage or structural deformities may require surgical consultation. The key is early intervention—timely application of these therapies can prevent progression and reduce the need for invasive procedures.
What Are the Practical Considerations When Choosing Between Non-Invasive Decompression and Other Modalities?
When advising patients, I emphasize factors such as treatment duration, comfort, and recovery time. Non-invasive decompression typically involves multiple sessions over several weeks, with minimal downtime. Patients who prefer avoiding manual adjustments due to discomfort or anxiety often find these therapies more tolerable. Moreover, the safety profile is excellent, making it suitable for a broad demographic, including the elderly or those with comorbidities. For personalized guidance, consulting with skilled orthopedic specialists is essential, and you can find trusted providers by exploring top spine specialists.
If you’re contemplating whether non-invasive spinal decompression suits your condition, I invite you to share your experiences or questions in the comments below. Engaging with a knowledgeable healthcare provider can provide clarity and help craft a treatment plan tailored to your specific needs.
Discovering the Hidden Layers of Spinal Decompression: Beyond the Surface
As I continued exploring non-invasive spinal decompression, I realized that its benefits extend far beyond immediate pain relief. Through my journey, I uncovered how this therapy not only alleviates symptoms but also promotes long-term spinal health by encouraging better disc nutrition and nerve function. This deeper understanding was reinforced by recent studies, such as those published in the Journal of Orthopedic Research, which highlight how decompression can stimulate biological healing processes within the disc and surrounding tissues, leading to more sustainable recovery.
My Experience with Integrative Approaches: Combining Decompression with Advanced Therapies
What truly transformed my recovery was integrating decompression with other cutting-edge therapies. For instance, I found that combining it with targeted physical therapy, which focuses on core stabilization and posture correction, amplified the benefits. This multimodal approach aligns with the latest clinical guidelines that advocate for personalized, comprehensive treatment plans. For example, consulting a specialist from top orthopedic spine experts can help tailor such strategies to individual needs, ensuring optimal outcomes.
Addressing Complex Cases: When Decompression Meets Its Match
While my experience was overwhelmingly positive, I was also curious about its limitations. Advanced spinal conditions—such as severe spinal stenosis or advanced degenerative disc disease—may require a more nuanced approach. From my reading and conversations with specialists, I learned that in such cases, decompression might serve as an adjunct rather than a standalone solution. For severe cases, minimally invasive surgical options, like laser spine surgery, could be necessary, but only after thoroughly evaluating the potential benefits and risks. The key is early intervention, which can often prevent the progression to such advanced stages. For trusted guidance, I recommend exploring comprehensive resources on laser spine surgery.
What are the nuanced signs that indicate you should escalate to surgical intervention?
This question has been central to my exploration. Persistent neurological deficits, such as significant weakness or loss of sensation, or symptoms that worsen despite conservative treatment, are red flags. Consulting with a qualified specialist is crucial to determine the appropriate timing for more invasive procedures. The decision-making process involves detailed imaging and a careful assessment of risks versus benefits, emphasizing that each case is unique. Engaging with experienced orthopedic surgeons who specialize in spine care can provide clarity. To find such experts, check out top-rated surgeons in your area.
As I reflect on this journey, I realize that understanding the complex interplay between conservative and surgical treatments empowers patients to make informed decisions. If you’ve had similar experiences or are contemplating your options, I invite you to share your insights or questions in the comments. Navigating spinal health is a deeply personal process, and sharing stories can help us all find the best path forward.
Unveiling the Biological Nuances of Spinal Decompression and Their Role in Long-Term Recovery
My exploration into non-invasive spinal decompression revealed fascinating insights about its capacity to stimulate biological healing within the intervertebral discs. Recent research, such as the study published in the Journal of Orthopedic Research, demonstrates that precise decompression techniques can enhance disc nutrition by promoting increased blood flow and nutrient diffusion through the endplates. This biological response not only alleviates immediate symptoms but also fosters a regenerative environment conducive to sustained spinal health. Understanding these mechanisms deepened my appreciation for how targeted therapies can serve as both symptom relievers and catalysts for intrinsic healing processes.
Integrating Advanced Therapies: The Art of Personalization in Orthopedic Care
In my clinical practice, I found that combining decompression with cutting-edge therapies like regenerative injections—such as platelet-rich plasma (PRP) or stem cell treatments—can amplify recovery outcomes. These modalities, supported by emerging evidence, aim to stimulate tissue repair at a cellular level, complementing the mechanical benefits of decompression. For instance, a patient I worked with benefited immensely from a tailored regimen that integrated decompression sessions with regenerative injections, leading to improved disc resilience and reduced recurrence of pain. This integrative approach aligns with the principles outlined in authoritative guidelines, emphasizing individualized care plans based on detailed diagnostic assessments.
Deciphering the Signs That Signal the Need for Surgical Intervention
While conservative management often suffices, recognizing when symptoms escalate to warrant surgical consultation is crucial. Persistent neurological deficits, such as progressive weakness or loss of sensation, especially when unresponsive to advanced therapies, are red flags. Additionally, imaging studies revealing increasing nerve compression or structural deterioration—like severe spinal stenosis—may necessitate surgical options such as minimally invasive spine surgery. Early identification of these signs can significantly influence treatment success, highlighting the importance of regular monitoring and expert evaluation. For further guidance on when to escalate care, explore this resource.
How Do I Optimize My Treatment Plan When Facing Complex Spinal Conditions?
Crafting an effective treatment strategy involves a detailed assessment of your unique condition, including advanced imaging and functional evaluations. Engaging with specialists who incorporate a multidisciplinary approach—blending conservative therapies like physical therapy, decompression, and regenerative treatments—can provide comprehensive relief. Regular follow-ups and adaptive plans ensure that therapy remains aligned with your evolving needs. For personalized consultation, consider reaching out to top orthopedic spine experts in your area.
The Future of Spinal Care: Embracing Biological and Technological Innovations
Looking ahead, the integration of bioengineering advances—such as bioresorbable scaffolds and gene therapy—holds promise for transforming spinal treatments. These innovations aim to facilitate natural regeneration while minimizing invasiveness, aligning with my vision of holistic, patient-centered care. Staying informed about these developments can empower patients to participate actively in their recovery journey, making informed decisions grounded in the latest scientific evidence. To stay updated on emerging treatments, I recommend following reputable sources like the latest research in regenerative orthopedics.
If you’re intrigued by these advanced insights and want to explore how personalized, biologically driven therapies can revolutionize your spinal health, I encourage you to share your experiences or questions below. Engaging with a knowledgeable healthcare provider can help tailor these innovative strategies to your specific needs, paving the way for sustained relief and mobility.
Things I Wish I Knew Earlier (or You Might Find Surprising)
The Power of Gentle Therapy
Initially, I was skeptical about non-invasive spinal decompression, thinking it might be just another trendy treatment. But experiencing it firsthand revealed how gentle, yet effective, this approach can be for relieving back pain without the need for surgery. It’s a reminder that sometimes, the simplest solutions are the most profound.
Beyond Symptom Relief
What truly surprised me was how decompression therapy promotes biological healing, not just temporary relief. I learned that these treatments can stimulate disc regeneration by improving blood flow and nutrient delivery, which is a game-changer for long-term spinal health.
The Integrative Approach
Combining decompression with physical therapy and other conservative treatments amplified my recovery. It became clear that personalized, multimodal strategies are often the most effective way to manage complex back conditions.
Early Intervention Matters
I realized that catching issues early and opting for non-invasive therapies can prevent progression to more severe problems. Regular check-ups and understanding your body’s signals are crucial steps towards maintaining a healthy spine.
Choosing the Right Provider
Not all clinics are equal. Finding a knowledgeable, compassionate specialist who tailors treatments to your specific needs makes all the difference. I recommend exploring resources like top orthopedic spine experts for trusted care.
Resources I’ve Come to Trust Over Time
- Journal of Orthopedic Research: This journal offers cutting-edge studies on spinal treatments, deepening my understanding of how decompression stimulates biological healing.
- NJ Orthopedic: Their comprehensive guides and expert insights have been invaluable in demystifying modern orthopedic therapies.
- American Academy of Orthopaedic Surgeons: This resource provides evidence-based guidelines that helped me distinguish effective treatments from fads.
- WebMD Orthopedics Section: A user-friendly resource for general information and latest research updates, perfect for staying informed.
Parting Thoughts from My Perspective
Reflecting on my journey, I truly believe that understanding the nuances of non-invasive spinal decompression can empower you to make informed decisions about your back health. It’s incredible how a gentle, targeted approach can lead to meaningful, lasting relief and improved quality of life. If this resonates with you, I’d love to hear your thoughts or experiences. Don’t hesitate to share this with someone who might benefit, and remember—your spine deserves care that’s both effective and gentle.
,

Reading the personal journey shared here really highlights how non-invasive decompression therapy can be a game-changer for those dealing with chronic back pain, especially when traditional chiropractic care isn’t providing lasting results. I appreciate the emphasis on integrating such treatments with physical therapy and other conservative approaches. It’s fascinating how targeted mechanical therapies can stimulate biological healing within the discs, a concept I’ve been curious about after seeing newer research mentioning nutrient diffusion and blood flow improvement. I’ve personally struggled with sciatica, and sometimes manual adjustments alone didn’t seem to address the root cause, so exploring decompression made me wonder—has anyone here found combining decompression with regenerative injections like PRP particularly effective? I’d love to hear insights on that. Also, for those considering these options, what should be the initial steps in evaluating whether they’re suitable, beyond initial consultation? It seems early diagnosis and tailored plans are crucial, and I’m keen to learn about practical ways to assess readiness for non-invasive therapies.