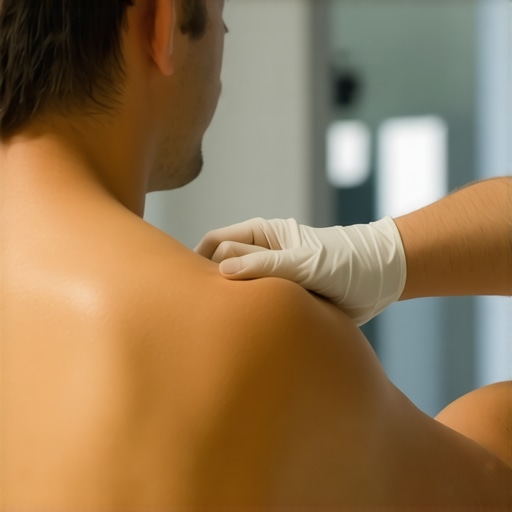
Have you ever woken up with a sharp pain in your shoulder that seemed to come out of nowhere? Maybe you tried to shrug it off, thinking it was just a pulled muscle from sleeping awkwardly or overusing your arm during everyday activities. But deep down, you knew something was off. That persistent ache, the limited range of motion, or the nagging discomfort—it’s enough to make you wonder: Am I really getting the correct diagnosis?
Why Understanding Shoulder Tests Matters in 2026
As someone who’s navigated the maze of orthopedic evaluations myself, I can tell you—getting the right assessment is half the battle. Especially now, where advancements in diagnostic techniques are reshaping how specialists pin down shoulder injuries. You might think, “Do I really need to go through a barrage of tests?” Well, here’s the thing: early, accurate diagnosis can make a huge difference in treatment outcomes.
In fact, according to recent studies, misdiagnosis or delayed diagnosis of shoulder issues can lead to prolonged pain and more invasive procedures down the line. Knowing what tests your NJ specialist will perform isn’t just medical paranoia—it’s empowering information that can help you advocate for yourself.
Have you faced these kinds of shoulder problems?
If so, you’re not alone. And I promise, understanding the upcoming tests can ease your mind and prepare you for what’s ahead. In this post, we’ll explore the five key assessments shoulder experts in New Jersey are expected to perform in 2026—tests that are designed to zero in on the root cause of your pain and guide the best course of action.
But be aware—making assumptions early on was a mistake I made. I once skipped a thorough exam, thinking a quick x-ray would suffice. That oversight delayed my recovery and led to unnecessary frustration. Trust me, a comprehensive evaluation includes a variety of examinations that go beyond the basics. Want to learn more about what to expect and how to prepare? Check out top orthopedic specialists in 2025.
Let’s dive into the tests that could hold the key to your shoulder health in 2026—and how they can help you avoid complications later on. Ready to discover what these assessments entail?
Prepare for the Examination
Start by noting any specific movements that trigger pain or weakness; this will help your orthopedic specialist understand your symptoms better. Wear loose clothing for easier access to your shoulder and arm, and arrive with a detailed history of your injury, including when it started and any activities that worsen it. Think of this initial phase as gathering the clues before solving a mystery, which sets the stage for targeted testing.
Understand the Key Physical Tests
Assess Range of Motion
Expect your doctor to evaluate both active and passive range of motion. Actively, you’ll move your shoulder in different directions; passively, the doctor will move your arm while you relax. This helps distinguish between joint, muscle, or nerve issues. Imagine it like testing a door’s hinges; if it swings freely, the problem might be inside the hinge mechanism, but if it resists, something’s wrong with the joint structures.
Strength and Stability Checks
The specialist will ask you to perform specific arm movements against resistance—like pushing or pulling—detecting weaknesses. These are analogous to testing a bridge’s support beams; weak points might indicate sprains or tears. I once tried this myself during a consultation; I was surprised how even mild weakness pointed to an underlying rotator cuff strain.
Specialized Shoulder Tests
Procedures like the Hawkins-Kennedy or Neer impingement tests mimic real-life motions that cause pinching pain. Think of these as controlled stress tests—similar to how engineers test bridges for load capacity—revealing hidden impingements or labral tears. For example, during my visit, the Neer test pinpointed an impingement even before an MRI was ordered.
Use Diagnostic Imaging to Confirm Findings
While physical tests provide valuable clues, imaging such as MRI or ultrasound offers detailed visuals of soft tissues like tendons and labrum. These scans are comparable to inspecting a building’s internal wiring; they expose issues that aren’t visible from external examination alone. My doctor recommended an MRI after inconclusive physical tests, which uncovered a partial rotator cuff tear, guiding effective treatment.
Integrate Testing Data for Accurate Diagnosis
Combine the physical exam results with imaging reports—like fitting puzzle pieces together—to reach a precise diagnosis. This holistic approach prevents misdiagnosis and ensures proper treatment. It’s similar to a lawyer analyzing evidence from multiple sources to build a compelling case.
Follow Up with Customized Treatment Plans
Once the diagnosis is clear, your specialist will craft a tailored plan—whether it’s physical therapy, nerve blocks, or minimally invasive surgery. Preparedness and understanding of the testing process empower you to engage actively in your recovery. For further insights into procedures like nerve blocks or orthopedic rehab, visit this comprehensive guide.
 Many people believe that understanding orthopedic diagnosis codes is straightforward, but the reality is far more complex. A frequent misconception is that these codes are merely bureaucratic tools, when in fact, they encode nuanced clinical information that impacts treatment pathways and insurance processes. For instance, misinterpreting a diagnosis code can lead to incomplete documentation in consultation notes, which might jeopardize legal cases or workers’ compensation claims. As an expert in orthopedic diagnostics, I’ve seen lawyers face hurdles due to overlooked nuances in these codes or mischaracterized examination findings.
Many people believe that understanding orthopedic diagnosis codes is straightforward, but the reality is far more complex. A frequent misconception is that these codes are merely bureaucratic tools, when in fact, they encode nuanced clinical information that impacts treatment pathways and insurance processes. For instance, misinterpreting a diagnosis code can lead to incomplete documentation in consultation notes, which might jeopardize legal cases or workers’ compensation claims. As an expert in orthopedic diagnostics, I’ve seen lawyers face hurdles due to overlooked nuances in these codes or mischaracterized examination findings.
A common myth is that all orthopedic evaluation notes are generic; however, detailed and precise documentation is crucial, especially for legal and insurance purposes. An improper note can delay proceedings or lead to denied claims, causing unnecessary frustration. For example, notes must accurately specify whether a nerve block was used as part of the management plan—something often misunderstood by non-specialists. Recognizing these subtle distinctions can make the difference between a successful claim and a costly denial.
Another trap is assuming that selecting between a spine surgeon and a chiropractor is an either/or decision. The truth is, each path offers distinct benefits depending on the nuances of your condition. A spine surgeon provides advanced surgical options for structural issues, while chiropractors may focus on conservative care. But, making this choice prematurely can lead to ineffective treatment if the diagnosis isn’t fully understood. Exploring whether a comprehensive assessment—including advanced imaging and physical tests—is necessary can help determine the right specialist. For instance, a thorough evaluation might reveal nerve impingement that only a spine specialist can address effectively. Check out this guide to making informed choices.
Focusing on workers’ comp cases, many assume that simple diagnoses suffice. Yet, complex injury cases often require specialized documentation and coding, such as complex orthopedic consultation notes tailored for legal clarity. These notes need to detail not only the diagnosis but also the functional limitations and treatment plans, especially for NJ workers’ compensation claims. Oversights here can delay settlement or proper coverage. To navigate this, understanding the finer points of orthopedic reports and how they tie into legal documentation is critical.
When considering orthopedic care for sports injuries, the nuance lies in differentiating acute management from long-term rehabilitation — what’s often overlooked is that orthopedic physical therapy involves more than just exercises. It includes manual therapy, soft tissue management, and modalities tailored to injury specifics. Knowing what’s included can help set expectations and improve outcomes. For example, prehab exercises can prevent future injuries, reducing your long-term downtime. Find out more here.
Regarding nerve block therapies, many believe they are a one-size-fits-all solution. But advanced orthopedic management considers patient-specific factors, the stages of nerve injury, and adjunct treatments that optimize outcomes. Misusing nerve blocks without proper evaluation can lead to dependency issues or mask deeper problems. A comprehensive understanding of nerve management strategies—such as combining nerve blocks with physical therapy—is essential. For more on this approach, visit this resource.
Finally, the hidden nuance often missed is the importance of detailed, accurate coding and notes for legal evidence. Overlooking small details can undermine your case or claim. Owners, lawyers, and patients alike must appreciate that these codes and documentation are a language—when mastered, they strengthen your position. Remember, continuous learning and attention to detail in this realm can save time and money.
Have you ever fallen into this trap? Let me know in the comments.
Maintaining optimal orthopedic health over the long term requires more than just visiting your doctor occasionally. It involves leveraging the right tools and methods that empower you to monitor, support, and enhance your recovery and prevention efforts daily. As someone deeply involved in orthopedic diagnostics and rehab, I’ve found specific equipment and software indispensable in my practice and personal regimen.
Smart Home Monitoring Devices for Post-Op Care
After surgeries like lumbar fusions or joint repairs, consistent monitoring is crucial. I recommend using wearable activity trackers like the Whoop Strap or Oura Ring. They provide real-time feedback on sleep quality, heart rate variability, and activity levels, which are vital metrics for preventing complications and detecting early signs of overexertion. These devices are personally used to track patient recovery progress remotely and adjust rehab plans accordingly, ensuring sustained improvements.
Advanced Imaging and Assessment Software
Incorporating software like OsiriX MD for DICOM image review helps clinicians analyze MRI and ultrasound images with precision. This technology enables detailed visualization of soft tissue changes over time, supporting decisions for ongoing management or scaling treatment. For example, tracking subtle rotator cuff repairs or nerve impingements becomes more accurate, thus optimizing long-term outcomes.
Digital Rehab Platforms
Tools like digital physical therapy platforms allow for guided exercises, remote clinician supervision, and progress tracking. I personally recommend PhysiApp because of its tailored programs that adapt to patient feedback and performance, helping prevent re-injury and boost mobility post-treatment.
Specialized Equipment for Desk Workers
Ergonomic tools—like adjustable sit-stand desks, lumbar supports, and ergonomic keyboards—are essential for preventing desk-related injuries. Personally, I use the Humanscale Liberty Sit-Stand Desk with a monitor arm that encourages posture shifts throughout the day. This proactive approach diminishes the risk of repetitive strain injuries and supports spinal health, especially for those with sedentary jobs.
Why These Tools Are the Future
As technology advances, integrating these tools into your routine will become even more seamless. Wearables with AI-driven health insights, cloud-based imaging analysis, and tele-rehab services are set to revolutionize long-term orthopedic management. Future trends suggest even more personalized, data-driven care options will emerge, making it easier to prevent injuries or catch issues early.
How do I maintain these tools over time?
Regular updates and calibration are key. Keep your devices synchronized with the latest firmware to ensure accurate readings. Schedule periodic reviews with your orthopedic specialist to interpret data and refine your care plan accordingly. Building this tech-supported approach into your routine not only amplifies the effectiveness of traditional treatments but also empowers you to take control of your health journey.
For dedicated guidance on integrating advanced tech into your rehabilitation, explore this resource. Remember, the key is consistency—embrace these tools as part of your daily routine for sustained orthopedic well-being.
Interested in adopting a new device or software? Consider trying the Whoop Strap for comprehensive recovery tracking and see how close you are to maintaining optimal orthopedic health.

My journey through shoulder pain taught me that the most profound insights often come from the smallest details in diagnostics. The real lesson wasn’t just about performing tests; it was about understanding the stories each patient’s body tells through subtle signs and nuances. Recognizing these clues early transformed my approach from reactive to proactive, saving many from unnecessary procedures and prolonged suffering. When I finally grasped that every test — from range of motion to specialized impingement assessments — was a piece of a larger puzzle, the entire picture of shoulder health became clearer, guiding me toward more effective, personalized care.
This revelation underscored the importance of not just trusting standard protocols but digging deeper into diagnostic subtleties. It’s about asking, ‘What’s this test really revealing? How does it fit into the bigger picture of a patient’s unique injury?’ Embracing this mindset shifted my entire practice, inspiring me to seek continuous learning, refine my skills, and truly listen to my patients’ bodies. Now, understanding orthopedic diagnosis codes and detailed examination notes isn’t just administrative; it’s a strategic advantage that empowers better patient outcomes, especially when navigating complex legal or insurance scenarios.
For those of us committed to excellence in shoulder care, staying ahead means embracing innovative assessments and honing our interpretive skills. The future belongs to providers who see beyond the surface, integrating advanced imaging with keen clinical insight. If you’re wondering whether a nerve block or a specialized test might reveal what’s not immediately visible, remember: it’s often the unseen details that hold the key to healing.
Embark on this journey with curiosity and confidence—your patients will thank you for it. And if you’re ever unsure about which diagnostic pathway is best, consult trusted resources like top specialists in New Jersey who combine innovation with personalized care.